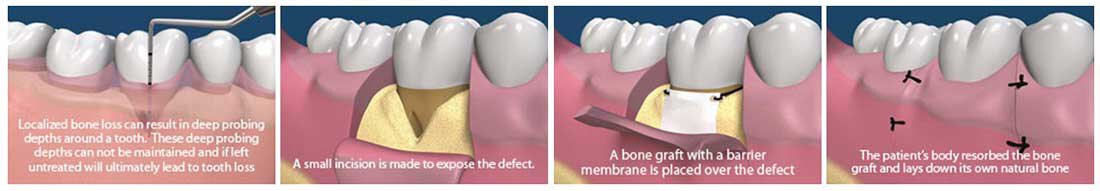
The goal of our Roseville periodontal therapy is to stop the progression of gum and bone loss and get your mouth to a healthy state. The initial stage of treatment is typically scaling and root planing to remove bacteria and calculus from below the gum line.
While this is an important step in the road to periodontal health, several studies have shown that it is virtually impossible to remove all the plaque and bacteria from pockets that are 5 mm and deeper. When deep pockets between teeth persist following this initial therapy, it is difficult for dental professionals and patients alike to keep these pockets bacteria and calculus free. Due to this, surgery is often necessary to restore periodontal health.

Depending on the topography of the bone defects, either a resective therapy (osseous surgery) or regenerative therapy (guided tissue regeneration) will be recommended by one of our specialist periodontists.
Resective therapy, termed osseous surgery, is often recommended when pockets are too deep to clean with daily home care and a professional care routine. Typically this is the case when pockets following scaling and root planning are still 5 mm in depth or greater. During this procedure, after administering anesthetic, the our Roseville periodontist pushes back the gum tissue and removes disease causing bacteria and calculus.
In most cases, irregular surfaces of the damaged bone are smoothed to limit areas where disease causing bacteria can hide. This reshaping of the bone allows for the gum tissue to reattach to the tooth after healing at a lower level down the root surface, reducing the pocket depth and improving the health of the affected teeth. The gums are then placed back over the newly shaped bone and sutured in place. Typically no antibiotics are prescribed for this treatment and over-the-counter pain medication is sufficient for any post-operative discomfort.
Curious if you need dental surgery on gum tissue? Contact one of our dentists today and schedule a consultation.
Gum surgery should be considered part of an overall strategy to stop periodontal disease from advancing, so healing can take place.
This 91 year-old gentleman presented to our periodontist on referral from his general dentist for “deep pocket depths that didn’t shrink after scaling and root planing.” Although osseous surgery was completed in all four quadrants of his mouth, we will focus on the upper right quadrant.
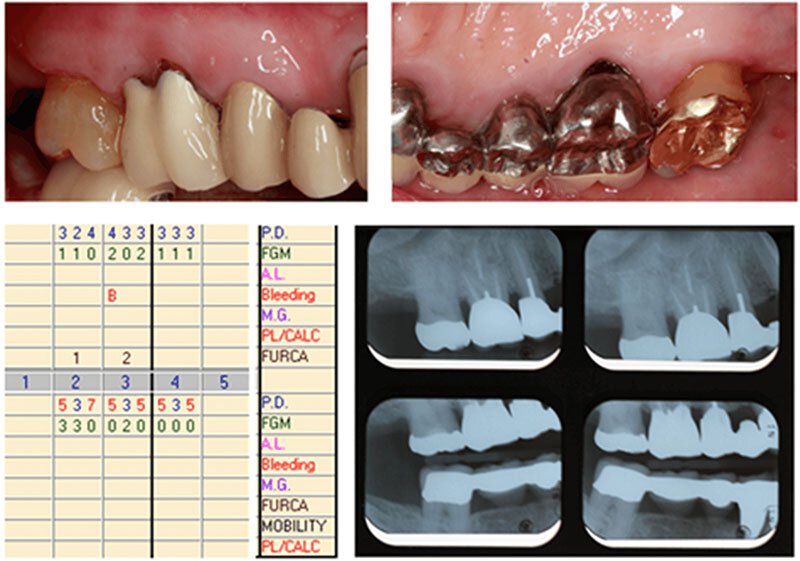
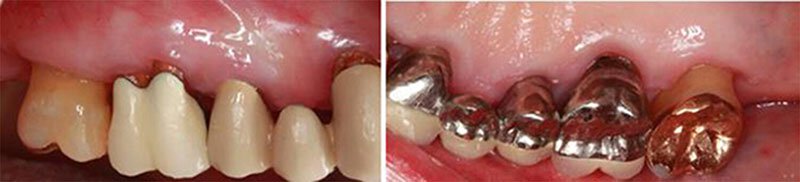
Osseous surgery was completed to reduce the 5-7 mm pockets and smooth out the defects, or holes, in the bone caused by periodontitis. The after surgery photo was taken 2.5 months following osseous surgery. Notice the improved health of the gum tissue.
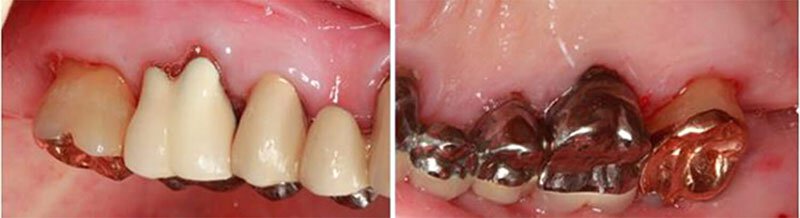
Photos taken one year post surgery. (At periodontal maintenance appointment)
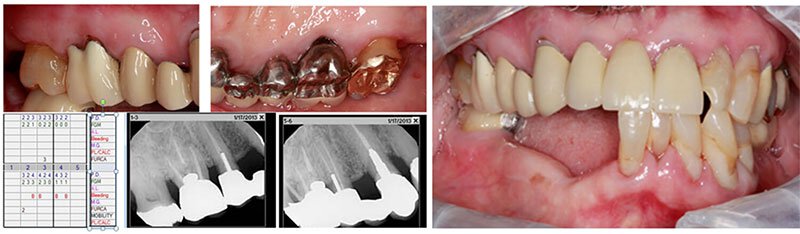
These photos, x-rays, and periodontal charting below were taken two years after surgery (at the patient’s periodontal maintenance appointment). Note that all pocket depths have remained less than 5 mm and his gum health has vastly improved and stayed healthy two years following osseous surgery.
With regenerative dental surgery Roseville dentists at Whole Dental have the goal to create an environment where the body rebuilds structures lost due to the disease process that attach a tooth to the jaw, including the bone.
This therapy is recommended when the pattern of bone loss is more vertical in nature, creating deep crevices within the bone surrounding teeth. If this therapy is recommended, after ensuring you are comfortably numb, your periodontist will gently push back your gums from the affected tooth (or teeth) and thoroughly clean out the deep pocket(s). Next, instead of smoothing out the defects in the diseased bone, the defects (or holes) are filled with a bone graft material and then covered with a membrane (like a fancy band-aid). The gums are then re-positioned over the affected site and sutured. Over the next six months to one year, your body will replace the grafted bone with your own new, natural bone and gum tissue, effectively increasing the support for that tooth and improving its lifespan. Typically antibiotics are prescribed for this treatment and over-the-counter pain medication is sufficient for any post-operative discomfort.
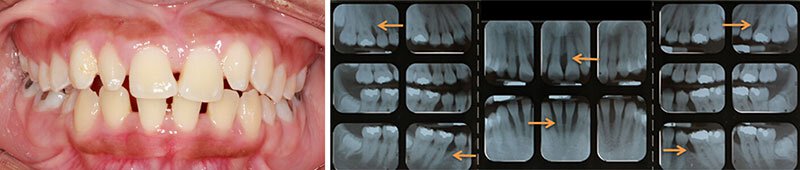
This 14 year-old female patient with localized aggressive periodontitis, a rapidly destructive form of periodontitis that causes severe bone loss around the front teeth (incisors) and first molars.
Notice how just looking at the patients gums, you may not guess that disease is present. Our team determined that the patient needed regenerative therapy on all four of her first molars to treat the severe bony defects. After all surgeries were completed, this patient was seen every 3 months for periodontal maintenance therapy and after 1.5 years, it was determined her gums and bone were healthy enough to allow her to get braces!
This 41 year-old male was referred to our periodontal team for evaluation and treatment of deep pockets that did not shrink after scaling and root planing was completed.
The first photo is the patient’s first visit to see our team. Although guided tissue regeneration was completed in multiple areas throughout the patient’s mouth we will focus on the lower right molar region. Note the severe bone loss and deep pockets on the first and second molar.
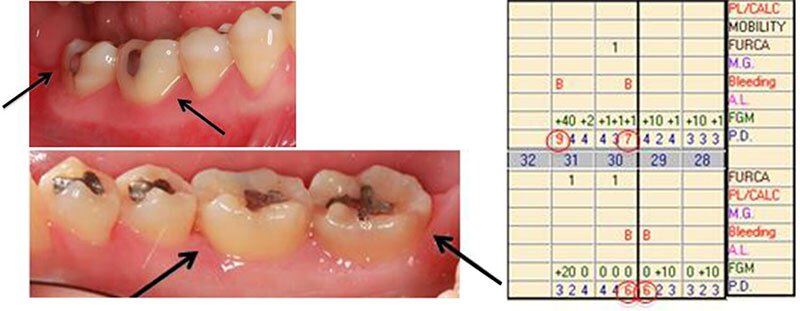
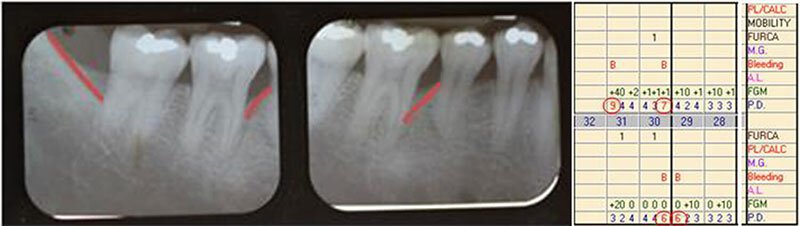
Guided tissue regeneration was performed on the front side of the lower right first molar and back of the second molar. X-rays were taken 6 months after regenerative therapy. At this point, the patient was placed on 3 month periodontal maintenance. This photo is prior to grafting.
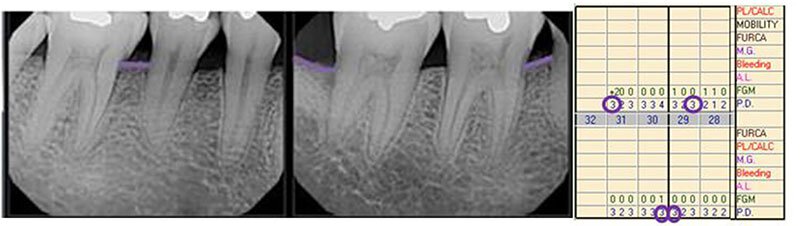
6 months post grafting.
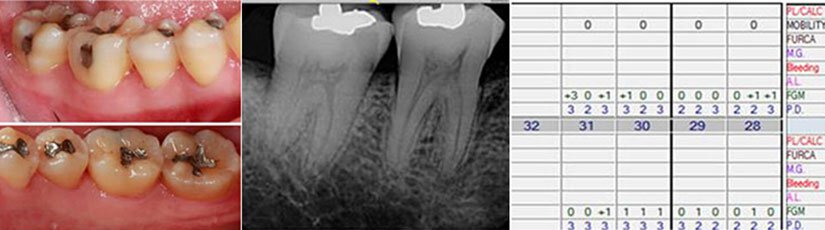
Radiographs, photos, and measurements taken 1.5 years post grafting which showed the stability of the graft and achievement of healthy bone and gums in this region. At this point, all pockets were less than 5 mm deep with no bleeding spots and healthy gum tissue. The patient was thrilled he was able to keep his teeth and with regular periodontal maintenance and good at home oral hygiene he should be able to keep them for his lifetime.
Contact our office today to request an appointment or fill out the form to book online. A team member will reach out to confirm your appointment.
21055 12 Mile Road, Roseville, MI 48066