Gingival recession is the exposure of the roots of teeth caused by loss of gum tissue and/or retraction of the gum margin away from the crown of the tooth. When recession occurs, the body loses a natural defense mechanism against bacterial penetration and trauma (often from your toothbrush!). Sometimes, when only minor recession is present and some healthy gum remains to protect the tooth, no treatment other than modifying home oral hygiene is necessary. However, when gum recession becomes a problem, soft tissue augmentation is an option to repair lost and damaged tissue.

With our cosmetic periodontal surgery Roseville patients have the ability to correct recession, which can often be unattractive.
This is especially important when the gums are visible when talking or smiling. Recession may cause your teeth to look longer than others and, in some cases, an exposed tooth root can cause severe pain because the root is exposed to extremes in temperature from different types of foods and liquids.
If only a few teeth are affected in a particular area, often a sub-epithelial connective tissue graft is the recommended treatment of choice. However, if several teeth in a particular area or an entire dental arch is affected, the use of acellular dermal matrix may be recommended. For more information on this product please visit: The Use of PerioDerm™ for Root Coverage and Correction of Insufficient Attached Gingiva
Once the cause of the recession, or defect, is determined, cosmetic periodontal surgery can repair the defect, correct pain and/or sensitivity, and help prevent further recession and bone loss.
Our Roseville periodontists are familiar with the latest techniques for diagnosing and treating periodontal disease, and also trained in performing cosmetic periodontal procedures.
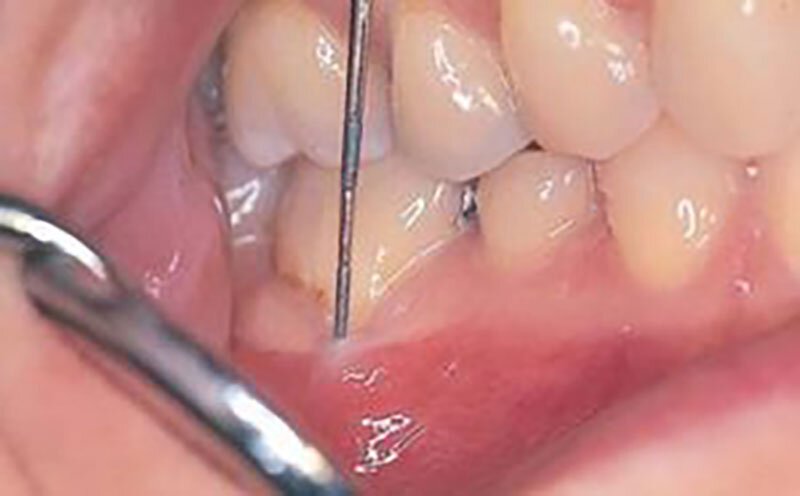
A sub-epithelial connective tissue graft is still the gold standard for correcting gingival recession and achieving root coverage on an affected tooth.
After ensuring you are comfortably numb, the recipient site (the tooth with recession) is prepared to receive the graft. Next, a piece of connective tissue is harvested from the roof of your mouth. After this piece of tissue is removed, the donor site is sutured closed. The piece of connective tissue is then positioned on the affected root surface and sutured into place. The existing gums are then pulled up over the top of the connective tissue graft to help protect it during healing and dissolving stitches are placed. Typically, no antibiotics are prescribed for this surgery and minimal post-operative pain medication is needed.
A gingival graft is designed to re-establish a zone of thick, healthy, attached gum tissue surrounding a tooth or dental implant. A thin piece of tissue is taken from the roof of the mouth, or gently rotated from an adjacent area where thick, healthy tissue is present, to provide a band of thick, healthy, attached gum around the affected tooth or dental implant. Oftentimes this procedure not only protects your tooth or implant from further gum and bone loss, but also improves the appearance the tooth!
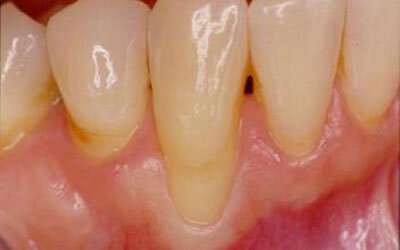
This patient presented to our periodontist with localized recession caused by a previous chin piercing. 3 month post-surgical photo showing correction of gum recession and thickening of tissue by placement of a gingival graft
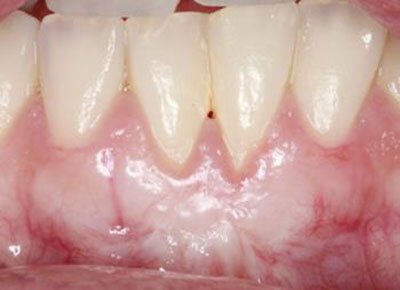
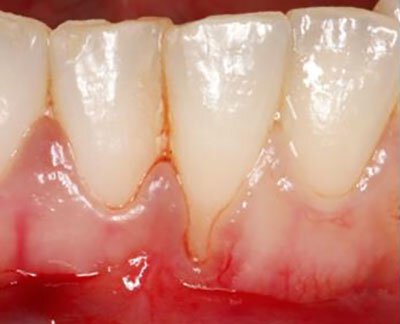
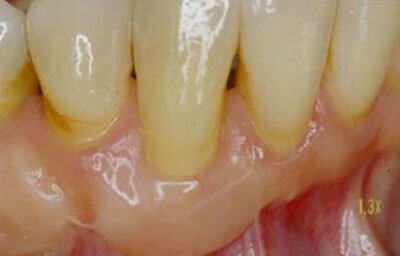
This patient was referred to our specialist periodontist to evaluate a localized area of gingival recession that was giving her extreme sensitivity to cold. Photograph taken 2 months post graft showing correction of defect.
Contact our office today to request an appointment or fill out the form to book online. A team member will reach out to confirm your appointment.
21055 12 Mile Road, Roseville, MI 48066